Many of us PIRCers came out of NIH-funded ELSI training programs, so we’re proud to have our individual and collaborative ELSI work represented at this year’s ELSI Congress at the Jackson Labs in Farmington, Connecticut.
PIRC at ACOG 2017

Megan Allyse is representing PIRC at the 2017 annual meeting of the American Congress of Obstetrics and Gynecology (ACOG) in San Diego, with a poster presenting preliminary findings from the ERRORS (Errors in Reading and Reporting On Results of Screening) study. She presented the ERRORS poster, titled “Decisional Regret in Women Receiving High-risk or Inconclusive Results from Non-invasive Prenatal Genetic Screening,” in ePoster Session B on Saturday (Poster 24B).
She is also presenting a poster on ethical considerations in uterine transplantation surgery, in ePoster Session P on Tuesday (Poster 30P). Congratulations Megan!
Mandating designer babies?
Technology for genetic modification has leaped forward in the past few years–thanks largely to the discovery and development of CRISPR, a new method of using bacterial enzymes to target and precisely cut DNA. In the wake of these developments, a recent article in The Atlantic asks, “Will Editing Your Baby’s Genes be Mandatory?” The article argues that as gene “editing” becomes safer and more reliable, modifying the genome of a fetus will eventually become commonplace, and parents who don’t utilize this option will be accused of endangering their child’s health. Continue reading Mandating designer babies?
PIRC at ACMG 2017
 We had a great time at the 2017 meetings of the American College of Medical Genetics and Genomics (ACMG), in Phoenix, Arizona. ACMG is a great meeting to learn about new and ongoing issues in medical genetics, including the many new developments in prenatal genetics that are important to our research group.
We had a great time at the 2017 meetings of the American College of Medical Genetics and Genomics (ACMG), in Phoenix, Arizona. ACMG is a great meeting to learn about new and ongoing issues in medical genetics, including the many new developments in prenatal genetics that are important to our research group.
Prenatal genetics in global context

We’re thrilled to announce the publication of our article summarizing insights from our Brocher Foundation workshop! In December 2015, we held a workshop at the Brocher Foundation in Geneva, Switzerland, on “Non-Invasive Prenatal Testing in the Non-Western Context.” With the participation of experts from around the world, we spent four days learning about the diverse social, economic, political, and cultural contexts in which prenatal cfDNA screening is being introduced globally, and discussed approaches to promote equitable and socially appropriate implementation. Our new article, published in the Hastings Center Report, shares 8 key insights emerging from that workshop.
Genetic counselors, genetic interpreters, and conflicting interests
by Katie Stoll, Amanda Mackison, Megan Allyse, and Marsha Michie
The booming genetic testing industry has created many new job opportunities for genetic counselors. Within commercial laboratories, genetic counselors work in sales and marketing, variant interpretation, as “medical science liaisons” to clinicians, and providing direct patient care. Although the communication skills and genetics expertise of the genetic counselor prepare them well for these roles, they also raise concerns about conflicts of interest (COI).
Continue reading Genetic counselors, genetic interpreters, and conflicting interests
Are We Ready For This?
Genetic counselor Robert Resta offers a critique of prenatal screening’s “mission creep” and lays out the things that should be in place–but aren’t–in order to support informed choices about prenatal screening.
Recent advances in genetic testing technology have us poised on the brink of a new paradigm of prenatal diagnosis – prenatal screening for all genetic and chromosomal conditions. Okay, not all disorders, but lots. Non-invasive Prenatal Testing (NIPT), whole exome sequencing, and expanded carrier screening are close to being available and affordable to a large proportion of the population. This is the culmination of a trend that began with the introduction of amniocentesis in the late 1960s, followed by ultrasonography, maternal serum screening, microarrays, and cell free placental DNA in maternal serum. From a strictly technical standpoint, each technology, while far from perfect, was an improvement on its predecessors in terms of accuracy, detection, false positive rates, and the range of detectable genetic conditions.
On the surface, this sounds like progress, and it is, in many ways. These technologies can contribute to the reduction of the incidence genetic conditions, some of which…
View original post 1,403 more words
Bioethics proposal for prenatal whole genome sequencing raises lively debate

The latest issue of the American Journal of Bioethics includes a target article by Stephanie C. Chen and David T. Wasserman entitled, “A Framework for Unrestricted Prenatal Whole-Genome Sequencing: Respecting and Enhancing the Autonomy of Prospective Parents.” As you might imagine, several PIRC members were prompted to submit open peer commentaries in response, so PIRC is well-represented in this lively debate, as you can see: Continue reading Bioethics proposal for prenatal whole genome sequencing raises lively debate
Having a child with Down syndrome is less expensive than many think
A study published today in the American Journal of Medical Genetics Part A finds that out-of-pocket medical costs of having a child with Down syndrome average less than $100 a month over the first 18 years of life. The study compared both out-of-pocket and insurance-covered costs for children with Down syndrome and matched peers without Down syndrome and found that, over the first 18 years, the additional medical costs of having a child with Down syndrome averaged $18,248 for families and $230,043 for insurers.
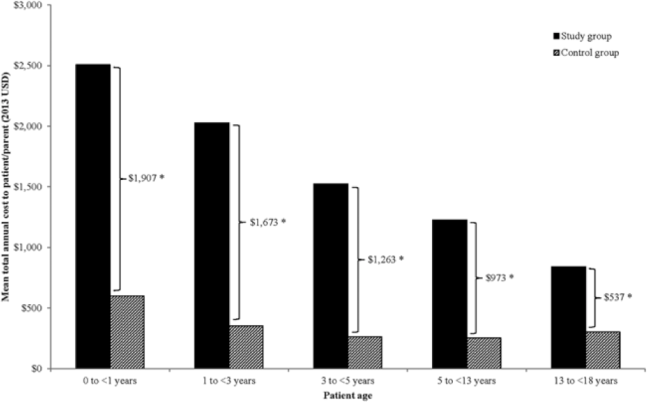
The authors found that medical expenses were highest in the first year of life, when children with Down syndrome are most likely to need surgeries that require a hospital stay. However, the average additional cost to families is perhaps surprisingly low, given the perception that children with Down syndrome incur burdensome medical costs. “I think many people will be surprised to learn that parents have few extra medical expenses when raising a child or adolescent with Down syndrome, since health insurance covers most of the costs,” said Dr. Brian Skotko, director of the Massachusetts General Hospital (MGH) Down Syndrome Program and a co-author of the study, in a MGH press release. “I hope our findings can help families better prepare for their own financial futures.”
For more information about life with Down syndrome, see the MGH Down Syndrome Program website, or download free materials at lettercase.org.
Recent developments in prenatal genetic testing
Here in the USA, where most of our PIRC collaborators reside, we’ve been pretty preoccupied lately with elections and such. But while we were doing other things, prenatal genomics has continued to produce new research and developments. Here are a couple of them.
Continue reading Recent developments in prenatal genetic testing
